Introduction
Inpatient mental health treatment gives people a structured, supervised setting to stabilize serious psychiatric symptoms when outpatient care is no longer enough. This guide covers who qualifies, what to expect from admission through discharge, how different programs work, and how to prepare yourself or someone you love. By the end, you will know exactly what steps to take next.
Quick Answer: Inpatient mental health treatment is a short-term, hospital-based level of care where patients receive 24-hour psychiatric monitoring, medication management, individual therapy, and group counseling. Most stays last 3 to 10 days, with the primary goal being stabilization before transitioning to a lower level of care.
What Is Inpatient Mental Health Treatment?
Inpatient mental health treatment is a form of intensive psychiatric care delivered inside a hospital or dedicated mental health facility. Patients stay on-site around the clock.
It differs from outpatient therapy because the patient sleeps, eats, and receives treatment all in the same building. Staff monitor symptoms continuously. This 24/7 structure makes inpatient mental health treatment appropriate for situations that cannot be safely managed at home.
The program combines medication evaluation, psychiatric assessment, individual therapy sessions, and structured group therapy. A psychiatrist leads the clinical team, supported by nurses, social workers, and mental health technicians.
Who Needs Inpatient Mental Health Treatment?
Inpatient mental health treatment is designed for people experiencing a psychiatric crisis. Not every difficult mental health moment requires hospitalization, but certain situations do.
Common reasons people enter inpatient mental health treatment include:
- Active suicidal ideation with a plan or intent
- Suicide attempt within the past 24 to 72 hours
- Severe psychosis with loss of contact with reality
- Manic episodes with dangerous or erratic behavior
- Inability to care for basic needs like eating or hygiene due to depression
- Severe withdrawal from substances combined with co-occurring psychiatric symptoms
A licensed clinician, an emergency room physician, or a crisis team typically makes the formal decision. In some states, an involuntary hold (sometimes called a 5150 or 302 hold, depending on the state) can admit someone without their consent when there is imminent danger.
If you are supporting someone who shows these signs, you can read more about involuntary psychiatric holds and what the process involves.
Types of Inpatient Mental Health Treatment Programs
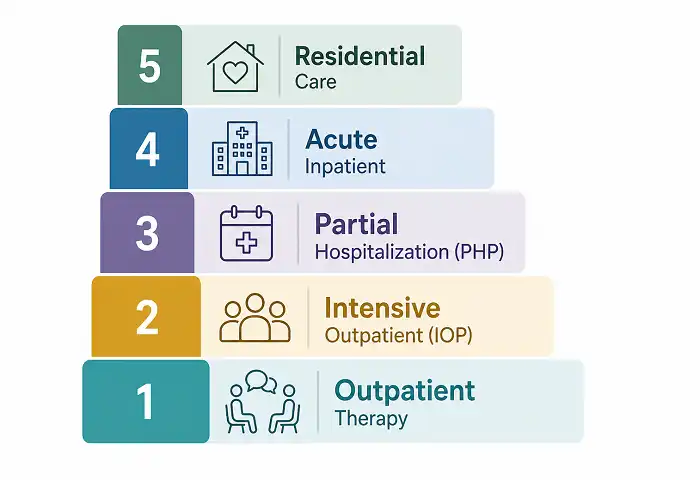
Not all inpatient mental health treatment looks the same. Facilities structure their programs differently depending on the patient population and severity of illness.
Acute Inpatient Psychiatric Units
These units sit inside general hospitals or stand-alone psychiatric hospitals. They focus on rapid stabilization. The average stay is short, typically 5 to 7 days.
Residential Mental Health Programs
Residential programs run longer, sometimes 30 to 90 days. Patients still live on-site, but the program emphasizes longer-term recovery, skill-building, and therapeutic milestones rather than just crisis stabilization.
Dual-Diagnosis Inpatient Programs
These programs treat co-occurring substance use disorder alongside the primary psychiatric diagnosis. Standard inpatient mental health treatment programs may not have the licensed addiction staff or medical detox capacity to handle both conditions simultaneously.
Child and Adolescent Inpatient Units
Separate units serve minors. Staff have specialized training in developmental psychology. Family therapy is a core component because parents and guardians are directly involved in the treatment plan.
What Happens During Inpatient Mental Health Treatment?
Day One: Admission and Assessment

The first day focuses entirely on evaluation. A psychiatrist or attending physician reviews medical history, current medications, and the presenting crisis. Blood work and a physical exam rule out medical causes for psychiatric symptoms.
Staff assign a safety level, which determines how closely the patient is monitored. Higher-risk patients receive one-to-one monitoring, meaning a staff member stays within arm’s reach at all times.
Daily Structure

Inpatient mental health treatment runs on a firm daily schedule. Structure itself is therapeutic because it reduces uncertainty and gives patients a predictable routine.
A typical day looks like this:
- Morning vitals and medication administration
- Breakfast with other patients in a communal space
- Morning group therapy session (topics vary: coping skills, emotion regulation, psychoeducation)
- Individual therapy or psychiatric check-in
- Lunch
- Afternoon group session or activity therapy (art, movement, journaling)
- Visiting hours, if permitted
- Evening group or recreational time
- Nightly medication round and lights out
Each day, the treatment team reviews progress in a brief team meeting. Medication adjustments happen frequently in the early days.
Medication Management
One of the core functions of inpatient mental health treatment is adjusting or initiating psychiatric medications under close supervision. Starting a new antipsychotic, mood stabilizer, or antidepressant in an inpatient setting lets clinicians monitor for adverse effects in real time.
According to general psychiatric guidelines from SAMHSA, medication decisions in inpatient care should involve the patient in a shared decision-making process whenever clinically possible.
Therapy During Inpatient Care
Group therapy is the backbone of inpatient mental health treatment. Individual sessions happen but are usually brief, 30 to 45 minutes, because the primary goal at this level of care is stabilization, not deep trauma processing.
Common therapeutic approaches used include:
- Cognitive Behavioral Therapy (CBT) to challenge distorted thinking patterns
- Dialectical Behavior Therapy (DBT) skills for emotion regulation and distress tolerance
- Motivational Interviewing for patients with co-occurring substance use
How to Prepare for Inpatient Mental Health Treatment
Preparing reduces anxiety about the unknown. Whether this is your own admission or someone you care about, a few practical steps make the transition smoother.
Documents to bring:
- Insurance card and photo ID
- List of current medications with dosages
- Emergency contact names and numbers
- Advance directive or psychiatric advance directive, if you have one
Items most facilities allow:
- Comfortable, loose-fitting clothing (no drawstrings or belts)
- Books or journals
- Personal hygiene items without alcohol content
Items most facilities prohibit:
- Phones and electronics (policies vary by unit)
- Sharps of any kind
- Prescription medications brought from home (the facility dispensary manages all medications)
Talking to someone who has gone through inpatient mental health care and recovery can help set realistic expectations before admission.
How Long Does Inpatient Mental Health Treatment Last?
The length of inpatient mental health treatment depends on the severity of the crisis, the patient’s response to treatment, and insurance coverage.
Most acute inpatient mental health treatment stays run 3 to 10 days. Longer stays require documented clinical justification, and insurance companies conduct utilization reviews to assess whether continued inpatient care is medically necessary.
Residential programs, which are a distinct level of care from acute inpatient, can run 30 to 90 days or more.
Discharge happens when the treatment team determines that the patient is no longer a danger to themselves or others, symptoms have stabilized, and a safe discharge plan with follow-up care is in place.
What Conditions Does Inpatient Mental Health Treatment Address?
Inpatient mental health treatment serves a wide range of psychiatric diagnoses in crisis. The most common include:
- Major Depressive Disorder with suicidal ideation or severe functional impairment
- Bipolar Disorder during manic or mixed episodes
- Schizophrenia and other psychotic disorders during acute breaks
- Severe Anxiety Disorders, including panic disorder with inability to function
- Eating Disorders when medical instability accompanies the psychiatric symptoms
- Post-Traumatic Stress Disorder (PTSD) when symptoms escalate to crisis level
- Borderline Personality Disorder during self-harm crises
Each diagnosis receives a tailored treatment plan within the inpatient mental health treatment framework.
Inpatient Mental Health Treatment and Insurance Coverage
Most private insurance plans, Medicaid, and Medicare cover inpatient mental health treatment. The Mental Health Parity and Addiction Equity Act requires insurance plans that cover mental health benefits to cover them at the same level as medical and surgical benefits.
Still, prior authorization is common. The hospital’s admissions team typically handles this on your behalf during an emergency admission. For planned admissions, calling your insurer in advance reduces billing surprises.
For more information on navigating insurance for psychiatric services, you can review United Healthcare’s mental health coverage details as a practical reference point.
The Discharge Plan: What Comes After Inpatient Mental Health Treatment?

Discharge planning starts on day one of inpatient mental health treatment. The social worker on the team begins identifying aftercare resources almost immediately.
A solid discharge plan from inpatient mental health treatment includes:
- Step-down level of care – Most patients transition to a Partial Hospitalization Program (PHP) or Intensive Outpatient Program (IOP) rather than returning directly to weekly outpatient therapy.
- Follow-up psychiatric appointment – Scheduled within 7 days of discharge whenever possible.
- Medication continuity – A prescription to bridge the gap until the outpatient psychiatrist takes over.
- Crisis plan – A written plan the patient keeps that lists warning signs, coping steps, and emergency contacts.
- Community support connections – Peer support groups, NAMI resources, or community mental health center enrollment.
Skipping step-down care significantly raises readmission risk. The transition period right after inpatient mental health treatment is one of the most vulnerable windows in psychiatric recovery.
How to Find Inpatient Mental Health Treatment
Finding inpatient mental health treatment starts with knowing where to look.
SAMHSA’s National Helpline (1-800-662-4357) offers free, confidential referrals to local treatment facilities 24 hours a day, 7 days a week. This is one of the most reliable starting points.
Your primary care doctor can also provide referrals. Emergency rooms admit patients directly when a crisis is active. For non-emergency situations, calling your insurance company’s behavioral health line gets you a list of in-network facilities.
The SAMHSA treatment locator is a government tool that lets you search by location, insurance type, and services offered.
Common Questions About Inpatient Mental Health Treatment
Is inpatient mental health treatment voluntary or forced?
Most admissions are voluntary. Involuntary inpatient mental health treatment requires a legal hold process that varies by state and involves clinical evaluation and sometimes a court hearing for extended holds.
Can family members visit during inpatient mental health treatment?
Most facilities allow visiting hours. Some units restrict visits during the first 24 to 48 hours to allow the patient to stabilize. Family therapy sessions are often incorporated into the treatment plan after the first few days.
Will inpatient mental health treatment show up on a background check?
Medical records, including psychiatric hospitalizations, are protected by HIPAA. They do not show up on standard employment background checks. Some security clearance processes involve direct disclosure questions, which is a separate matter.
Does inpatient mental health treatment actually work?
Research consistently shows that inpatient mental health treatment reduces immediate crisis risk and improves short-term outcomes when followed by structured aftercare. It is not a cure, but it is an effective intervention point when someone’s safety is at risk.
If you are exploring what mental health support looks like across the full spectrum, understanding what a mental health check-in involves can help you identify earlier warning signs before a crisis escalates.
Mistakes to Avoid With Inpatient Mental Health Treatment
Waiting too long. Many families wait until a crisis is severe before pursuing inpatient mental health treatment. Earlier intervention typically means a shorter, less traumatic hospital stay.
Leaving against medical advice (AMA). Patients have the legal right to leave voluntarily admitted inpatient mental health treatment, but leaving before the team considers it safe dramatically raises the risk of rapid deterioration.
Skipping aftercare. Inpatient mental health treatment addresses the acute crisis. Without follow-up PHP, IOP, or outpatient therapy, relapse into crisis is common within weeks.
Not being honest during intake. The assessment on day one shapes the entire treatment plan. Minimizing symptoms or hiding medication history gives the team incomplete information to work with.
Supporting Someone Through Inpatient Mental Health Treatment
If someone you love is in inpatient mental health treatment, your role matters. Ask the treatment team what family involvement looks like. Attend family therapy sessions if offered.
Avoid minimizing the experience when they return home. Phrases like “you seem fine now” or “just stay positive” can feel dismissive to someone who just went through a psychiatric hospitalization.
Instead, focus on logistics: driving them to follow-up appointments, helping them establish a routine, and learning their crisis plan so you can support it.
Many families find that connecting with mental health cooperative support resources helps them navigate the caregiver role with better tools.
You might also benefit from reading about how to find the right mental health match for ongoing outpatient care after discharge.
Conclusion
Inpatient mental health treatment saves lives. It gives people in crisis a safe place to stabilize, get the right medications, and build a foundation for recovery. The process can feel overwhelming from the outside, but knowing what to expect makes it less frightening.
If you or someone you care about is in crisis right now, call 988 (the Suicide and Crisis Lifeline) or go to your nearest emergency room. Inpatient mental health treatment is not a last resort; it is a legitimate, effective level of care for the moments when safety requires more than weekly therapy can provide.

